Macular Hole Surgery in Delhi
Home > Service Detail
Macular Hole Surgery in Delhi
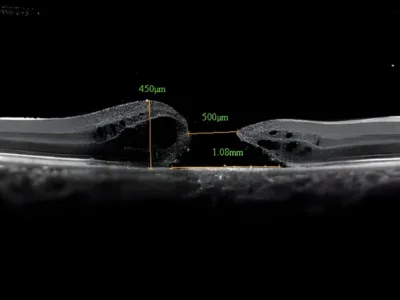
A macular hole is a small, full-thickness defect at the very centre of the retina — the macula — which is responsible for your sharpest, most detailed vision. When a macular hole develops, everyday tasks like reading, recognising faces, and driving become increasingly difficult. Left untreated, it can lead to permanent central vision loss.
At Claritas Eye & Retina Institute, one of the most trusted eye hospitals in Delhi, we have helped hundreds of patients restore their central vision through precise, minimally invasive vitreoretinal surgery. Our dedicated retina programme is built around a single goal: giving you the best possible visual outcome with the least possible disruption to your life.
Dr. Mayank Bansal says:
“A macular hole, when detected early, is highly treatable — but timing is everything. The longer a hole remains untreated, the more challenging recovery becomes. My priority is not just surgical success, but restoring the vision quality that lets my patients live fully.”
What Is a Macular Hole?
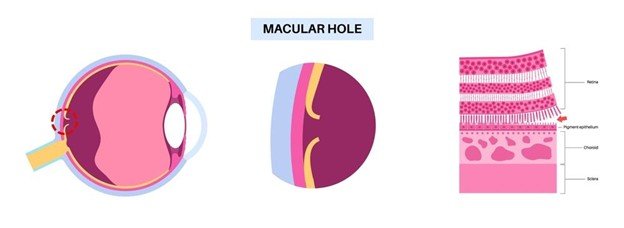
The macula sits at the centre of the retina and contains the highest concentration of photoreceptor cells in the eye. It allows you to see fine detail, read text, and perceive colour clearly. A macular hole occurs when the vitreous gel inside the eye pulls away from the macula abnormally, creating a tear or hole in this critical region.
Stage 1 — Foveal Detachment
Early stage where the centre of the macula begins separating. Vision may be only mildly affected. Close monitoring is advised.
Stage 2 — Partial Thickness Hole
A partial-thickness break forms at the fovea. Central blurring becomes noticeable. Early surgical intervention is recommended.
Stage 3 — Full-Thickness Hole
A complete hole forms across the macula. A central scotoma (dark spot) appears. Vitrectomy surgery is the standard treatment.
Stage 4 — Large Full-Thickness Hole
The vitreous has fully detached. The hole is larger and may require advanced surgical techniques for successful closure.
Causes
Age-related vitreous changes, high myopia, eye injury, retinal detachment, or chronic macular oedema can all contribute to hole formation.
Risk Factors
Age over 60, female sex, high myopia, history of eye trauma, or a macular hole in the fellow eye increases susceptibility.
Symptoms of a Macular Hole
Macular holes rarely cause pain, which is why many patients delay seeking treatment. Watch for these visual warning signs:
Distortion of straight lines (metamorphopsia)
Lines that should appear straight — door frames, text, tiles — appear wavy, bent, or irregular.
Dark or blind spot in the centre of vision
A grey or dark patch at the centre of what you’re looking at, making reading or face recognition difficult.
Difficulty reading fine print
Even with glasses, small text becomes hard to make out due to the central visual disruption.
Reduced colour perception
Colours in the centre of your visual field may appear washed out or less vivid than they used to be.
Gradual worsening of central vision
Unlike sudden vision loss, macular holes tend to worsen slowly over weeks to months if left untreated.
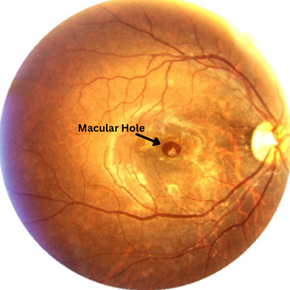
How Is Macular Hole Surgery Performed?
The standard and most effective treatment for a macular hole is a procedure called pars plana vitrectomy — a form of retina surgery in Delhi that Dr. Mayank Bansal performs routinely with exceptional precision. Here’s what the process looks like from your first consultation to recovery.
Step 1: Comprehensive Pre-Surgical Evaluation
A detailed OCT scan and dilated fundus examination assess the size, stage, and duration of the macular hole. This guides the surgical plan and helps set realistic visual expectations for recovery.
Step 2: Micro-Incisional Vitrectomy (MIVS)
Using 23- or 25-gauge instruments — thinner than a human hair — Dr. Bansal makes tiny incisions in the eye wall to access the vitreous. The gel is carefully removed to relieve traction on the macula.
Step 3: Internal Limiting Membrane (ILM) Peeling
A very thin, transparent membrane over the macula — the ILM — is delicately peeled away. This critical step removes residual traction and significantly increases the rate of hole closure.
Step 4: Gas Tamponade
A sterile gas bubble is injected into the eye to gently press the hole closed from inside. Patients are asked to maintain a face-down position for a period post-surgery to maximise the effect of the gas tamponade.
Step 5: Personalised Post-Operative Care
Regular follow-up appointments, medicated eye drops, and positioning advice are provided. Most patients notice gradual vision improvement over weeks to months as the macula heals and the gas bubble dissolves naturally.
Recovery and Aftercare
Recovery after macular hole surgery is a gradual process that requires patience and strict adherence to your surgeon’s instructions. Here is what to expect at every stage — and how our team at Claritas supports you throughout.
Face-Down Positioning (Days 1–14)
The most critical part of early recovery. You will be asked to maintain a face-down posture for 5–14 days post-surgery so the gas bubble remains in contact with the macular hole, pressing it closed. Special positioning pillows and equipment can be arranged to make this more comfortable.
Eye Drops & Medications
You will be prescribed antibiotic and anti-inflammatory eye drops to prevent infection and reduce swelling. These must be instilled exactly as directed — typically 3–4 times daily for 4–6 weeks. Do not stop drops without consulting Dr. Bansal.
No Flying Until Gas Bubble Dissolves
Air travel is strictly prohibited while the gas bubble is present inside your eye. Changes in cabin pressure can cause the bubble to expand dangerously, leading to a sudden spike in eye pressure. Your surgeon will clear you to fly once the gas has fully absorbed — usually 6–8 weeks after surgery.
Vision Changes in the First Few Weeks
Vision will initially be blurry and obscured by the gas bubble — this is completely normal. As the bubble slowly dissolves over 4–8 weeks, your vision will begin to clear. Most patients notice meaningful improvement from 4–6 weeks, with continued recovery over 3–6 months.
Activity Restrictions
Avoid strenuous exercise, heavy lifting, and bending at the waist for at least 4 weeks. Light walking is generally permitted from day 3 onwards. Swimming and contact sports should be avoided for a minimum of 6–8 weeks. Your care team will advise you on when to safely resume each activity.
Follow-Up Appointments & OCT Monitoring
Regular review appointments are scheduled at 1 week, 4 weeks, and 3 months post-surgery. OCT imaging is used at each visit to confirm hole closure and monitor macular healing. Remote follow-up is available for international and outstation patients.
Updated Glasses Prescription
Surgery often changes the refraction of the eye slightly. Wait until your vision has fully stabilised — typically 3–6 months post-operatively — before updating your spectacle prescription. Attempting an earlier refraction may yield an inaccurate result.
Why Choose Claritas Eye Hospital for Macular Hole Surgery in Delhi?
Choosing where to have your retinal surgery is a significant decision. Here’s why patients across Delhi — and from around the world — trust Claritas Eye & Retina Institute for their most complex eye conditions.
Internationally Trained Retina Surgeon
Dr. Mayank Bansal’s dual training at AIIMS and UCLA ensures you receive surgical care that meets global standards — right here in Delhi.
Advanced Micro-Incisional Vitrectomy
We use 23- and 25-gauge MIVS technology — the latest in minimally invasive retina surgery — for faster healing and minimal surgical trauma.

Dedicated Retina & Vitreous Programme
Unlike general eye hospitals, Claritas specialises in retinal conditions. Our entire infrastructure is purpose-built for retina care in Delhi.

High-Resolution OCT Diagnostics
State-of-the-art optical coherence tomography allows us to map your macula in extraordinary detail, enabling precise surgical planning.

Experienced with International Patients
We provide end-to-end support for patients travelling from abroad — including pre-op communication, surgery, and remote follow-up.

Transparent, Patient-First Communication
Dr. Bansal takes time to explain your diagnosis, surgical options, and recovery thoroughly. No rushed consultations, no hidden decisions.

FAQs
1. What is the success rate of macular hole surgery?
2. How long does macular hole surgery take?
3. What is the recovery time after macular hole surgery?
4. Do I need to maintain a face-down position after surgery?
5. Is macular hole surgery painful?
6. Is macular hole surgery painful?
Disclaimer: The information shared in this content is for educational purposes and not for promotional use.

 English
English
 العربية
العربية
 Русский
Русский
 Français
Français
 Español
Español
 বাংলা
বাংলা
 Kiswahili
Kiswahili
 Deutsch
Deutsch
 中文
中文
 日本語
日本語
 हिंदी
हिंदी
