Eye Surgery Safety in India for British and American Patients?
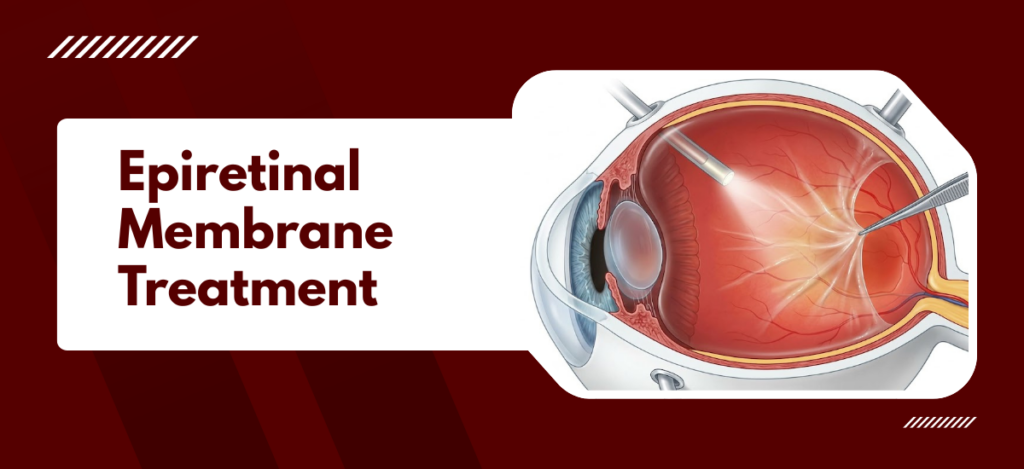
An epiretinal membrane is a thin layer of fibrocellular scar tissue that forms on the surface of the macula, the central part of the retina responsible for sharp, detailed vision. It is also called macular pucker or cellophane maculopathy. The membrane distorts central vision by contracting and pulling on the retina, causing it to wrinkle and bend, which makes straight lines appear wavy and produces blurred reading vision. Severity depends on membrane thickness, the strength of traction on the macula, and whether the foveal contour is disrupted on OCT imaging. Most cases are idiopathic and linked to age-related posterior vitreous detachment, while others follow retinal tears, diabetic retinopathy, uveitis, or prior intraocular surgery.
According to Dr. Mayank Bansal,Best Eye Hospital in Delhi, Not every epiretinal membrane needs surgery. The decision rests on documented vision loss, metamorphopsia on Amsler grid, and structural disruption visible on OCT, not on the membrane’s mere presence.
Symptoms vs Clinical Significance
Patient-Reported Symptom | Clinical Indicator | Severity Marker |
Wavy or bent straight lines | Metamorphopsia | Moderate to severe |
Central blur during reading | Foveal distortion on OCT | Surgical candidate |
Double vision in one eye | Monocular diplopia from traction | Advanced membrane |
Difficulty judging distances | Aniseikonia | Functional impairment |
Mild haze in central vision | Early cellophane reflex | Observation suitable |
What symptoms suggest an epiretinal membrane is forming?
Most patients ignore early changes because peripheral vision stays intact and the second eye compensates during daily activities. Cover-one-eye testing usually reveals the problem.
Distortion: Straight edges like door frames or text margins appear curved, and this remains the most reliable early indicator of macular traction.
Reading difficulty: develops gradually, with patients needing brighter light and larger fonts, and sometimes describing letters that seem to jump or shift on the page.
Size mismatch: One eye sees objects smaller or larger than the other, which is called aniseikonia and creates depth perception issues.
Central haze: that doesn’t clear with blinking, often described as looking through cling film or a smudged lens, separate from typical refractive blur.
Symptoms rarely improve without intervention once metamorphopsia is established and traction is documented on imaging. For deeper detail on related macular conditions, see our page on macular hole surgery in Delhi.
When is vitrectomy surgery recommended for macular pucker?
Surgery is reserved for symptomatic cases where vision drops below functional thresholds or distortion interferes with reading, driving, and daily work. Observation remains valid for mild, stable membranes.
Vision threshold: Best-corrected acuity dropping below 6/12, or rapid decline across consecutive visits, generally tips the balance toward intervention.
OCT findings: showing inner retinal thickening, ectopic inner foveal layers, or loss of foveal pit anatomy strengthen the surgical case, and these are reviewed alongside the procedure called vitrectomy surgery in Delhi during the planning stage.
Distortion severity: matters even when visual acuity is preserved, because patients with intolerable metamorphopsia often benefit from membrane peel.
Patient lifestyle: A retired person reading mostly large print may defer surgery, while a working professional with bilateral involvement usually proceeds sooner.
Membrane removal with internal limiting membrane peel under 25-gauge vitrectomy is the standard surgical technique. For a related read, see our guide on macular hole symptoms and treatment.
Visual Recovery Timeline After Vitrectomy
Postoperative Period | Expected Visual Status | Activity Guidance |
Week 1 | Blurred, gas bubble present if used | Rest, avoid lifting |
Weeks 2 to 6 | Gradual clearing, distortion reduces | Light desk work permitted |
Months 3 to 6 | Measurable acuity improvement | Most activities resumed |
Months 6 to 12 | Continued slow improvement | Final visual outcome assessed |
Why Choose Dr. Mayank Bansal?
Dr. Mayank Bansal trained at AIIMS New Delhi and completed advanced retina fellowships including ICO Retina Fellowship at UCLA, with FRCS Glasgow and FACS credentials backing 15-plus years of vitreoretinal practice. His surgical record includes thousands of complex retina procedures handled by Dr. Mayank Bansal personally rather than delegated to junior staff.
Patients consistently report measurable reduction in metamorphopsia within three months of membrane peel, and visual acuity gains of two lines or more in roughly seven out of ten eyes when surgery is timed correctly. Outcomes depend on how long traction has been present before intervention.
FAQ
Does epiretinal membrane go away on its own?
No, surgical removal is the only definitive treatment for symptomatic cases.
Will my distortion fully disappear after surgery?
Distortion reduces significantly but may not vanish completely in long-standing cases.
How long is recovery after macular pucker surgery?
Visual recovery typically continues over three to six months postoperatively.
Can epiretinal membrane recur after peeling?
Recurrence is uncommon when internal limiting membrane peeling is performed.

 English
English العربية
العربية Русский
Русский Français
Français Español
Español বাংলা
বাংলা Kiswahili
Kiswahili Deutsch
Deutsch 中文
中文 日本語
日本語 हिंदी
हिंदी